The Achilles tendon is the longest and strongest tendon in the human body. It plays a vital role in body movement and balance. Although the Achilles tendon is very robust and powerful, it is vulnerable to injuries such as ruptures. Here, we explain the possible symptoms and causes of an Achilles tendon rupture, as well as optional types of treatment.
Achilles tendon and Achilles tendon rupture – What is it?
The Achilles tendon is a strong and tear-resistant tendon between 15 and 25 centimeters long and up to 5 centimeters wide at its thickest point. It constitutes the end portion of the three-headed calf muscle and serves to attach it to the heel bone of the foot.
The tendon can withstand heavy physical stress – in extreme situations, for example, bearing ten times one’s body weight. In addition, the Achilles tendon is surrounded by the tendon sheath, which permits the tendon to glide over the bone almost unobstructed.
Among the most frequent injuries is an Achilles tendon rupture, inflammations and irritations. The likelihood of such a rupture occurs most frequently for persons aged 30 to 40 years. If the Achilles tendon is only slightly ruptured and not completely severed, this is known, medically speaking, as a partial tear.
Achilles tendon rupture: These symptoms are indicators
There are typical symptoms for an Achilles tendon rupture. In many cases, a whip-like popping sound or a sudden snap can be heard accompanied by a sudden onset of sharp pain in the heel. The injured person can then walk only with great difficulty. A further indication is no longer being able to walk on one’s toes and one’s foot can no longer roll on the ball of the foot.
In contrast to a complete Achilles tendon rupture, a slightly torn Achilles tendon is, in many cases, not easy to identify, as the pain does not occur as intensely and the person affected is frequently still able to walk normally. A partial tear is often identified only after a period of time, as severe pain in the Achilles tendon does not necessarily have to occur immediately.
Should an Achilles tendon tear occur, swelling on the back part of the ankle, as well as swelling of the lower thigh are common signs. In some cases, a bruise is formed above the ankle.
If the pain in the Achilles tendon area is suspected to be a rupture, then first aid needs to be administered immediately for a sports injury. The RICE approach is then to be deployed. In this case, the affected leg is to be elevated and rested. It is advisable to cool the joint cautiously, whereby the ice is not permitted to be placed directly on the skin. To avoid a freezing action, the ice needs to be wrapped in a cloth. A medical examination is then to be initiated as quickly as possible.
Causes of an Achilles tendon rupture
The cause of an Achilles tendon rupture is not due to an extreme forceful external impact, but rather by unexpected, intense physical stress – in most cases, the tendon has already been damaged previously as a result of excessive movements of the ankle and/or degenerative changes. An Achilles tendon rupture occurs most commonly during athletic activities involving sudden changes in direction, stops and starts, as well as fast sprints – typically for sports like basketball, handball or tennis. Whether or not a person is involved in sports actively, a rupture of a (previously damaged) Achilles tendon can easily occur when a sudden movement with excessive physical force is made.
The risk of having an Achilles tendon rupture is heightened if an inflammation of the tendon’s sheath (tenosynovitis) is present, as the tendon is thus irritated. Additional illnesses can also irritate the Achilles tendon and make a rupture more likely, for example, gout, arthrosis or diabetes mellitus.
Additional factors increasing the likelihood of an Achilles tendon rupture:
- Shortened musculature of the calf muscles
- Older age or weak physical condition
- Malposition of the foot
- Insufficient warm-up prior to sports
- Inappropriate footwear
- Recurring excessive physical stress during sports
Diagnosis for a rupture of the Achilles tendon
Should pain occur in the area of the Achilles tendon, it is essential to undergo an examination by a medical doctor. It is best to consult a specialist physician or an emergency surgery clinic – or, for immediate aid, to go to the accident and emergency (A&E) department.
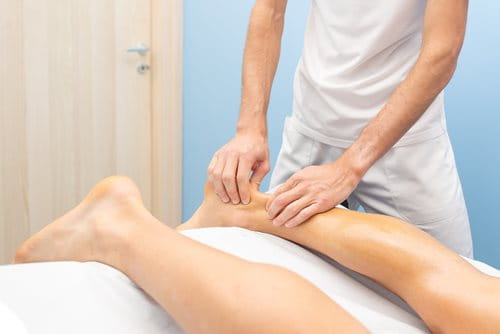
The attending medical staff will then first ask several questions in order to establish whether the injured person:
- is able to walk normally,
- perceived a sudden onset of symptoms,
- has already had similar ankle pains or injuries and
- can explain how the accident occurred.
The diagnosis can most often be made clinically by way of inspection and palpation (feeling). A few centimeters above the end of the heel bone (calcaneus), a gap in the tendon can be felt. In addition to palpation, the range of motion and ability to bear physical stress, as well as the muscle strength (toe standing on one leg) is tested.
A special clinical test for a suspected Achilles tendon rupture can also be deployed by medical staff, the so-called Thompson Test, also known as the ‘calf-squeeze test’. This examination entails having the patient lie face down on the examination table with one’s feet hanging off the edge of the table, so that the calf muscle of the injured leg can be squeezed. Normally the foot stretches (plantar flexion), but with a patient with a ruptured Achilles tendon, the foot will not move.
To confirm the diagnosis reliably, medical imaging can provide support by performing an ultrasound examination, for example. This is, above all, useful for providing evidence of a partial tear. The ultrasound allows the structure of the Achilles tendon to be clearly represented and, in the case of a (partial) tear, permitting a gap to become visible.
Achilles tendon rupture: Treatment
If examination results show that there is an irritation of the Achilles tendon, it is recommended that the ankle is not physically stressed. To support the joint, special bandages are well suited. Resting the foot should be ensured, otherwise the irritation may become chronic and, in turn, heighten the risk of an Achilles tendon rupture. Moreover, it is advisable to also treat the affected site by providing cooling.
But what to do if the Achilles tendon is completely ruptured? Should this be the case, there are then two options to consider: surgery and a conservative treatment.
Achilles tendon tear: Therapy without surgery
If a conservative therapy for a torn Achilles tendon is possible, the treatment is then without surgery. This means the patient is required to wear a cast around one’s calf, a splint (orthosis) or a special shoe with a slightly pointed foot position. The aim here is to have the severed tendon ends align closer to one another and to attain scarring in the course of the healing process.
Subsequently, a shoe or boot orthosis is to be worn for a time period of six to eight weeks. Based on the medical diagnosis and treatment, the pointed-foot position is gradually reduced step by step during the treatment period. Furthermore, measures are taken to prevent thrombosis from occurring. Physical therapy is a treatment measure to be deployed.
In principle, the conservative method is more arduous than having an operation. This is due to the Achilles tendon needing a great deal of rest and, above all, time to heal.
Achilles tendon rupture therapy: Surgery
The advantage of having surgery is that the tendon regains its ability to function much more quickly and the likelihood of an Achilles tendon rupture occurring again is lower. Nevertheless, an operation can result in complications, which need to be taken into account in a medical consultation prior to surgery.
The surgical therapy can be performed either as minimally invasive or as open surgery. In both cases, the tendon ends are stitched together. If the torn-off tendon is in such poor condition that simple sewing together is not feasible, then a piece of tendon from another part of the body is used or a special stitching technique is deployed. Generally speaking, there are numerous methods available for surgical procedures.
An Achilles tendon operation is performed using either regional or local anesthesia – general anesthesia is not necessarily required. During the operation, the patient lies face down, with one’s feet hanging down over the edge of the operating table. To achieve the optimal result, both feet are continuously observed and compared, with a focus on the sural nerve (nervus suralis). This sensitive nerve is located near the Achilles tendon and is not to be damaged, as it innervates the heel of the foot.
Following the operation, a lower-leg cast with pointed-foot positioning is to be worn for four to six weeks, during which time the pointed positioning is reduced every two weeks. After a surgical procedure, physical therapy is also to be provided.
To what extent sports activities can once again be performed should be decided in a consultation with a medical professional.
Achilles tendon rupture: How to minimize the risk
Normal wear and tear of the Achilles tendon cannot be prevented. However, the general risk of injury can be minimized, by doing the following:
- warming up one’s muscles properly before training / sports
- gradually increasing physical stress during sports
- using suitable footwear
- doing sports moderately
- not overly exerting your body and taking time after sports for regeneration.

Laura de Bruin graduated in 2013 as a physiotherapist at the Hogeschool Rotterdam. In September 2015 she started the Master's degree in Manual Therapy in Rotterdam. In June 2018 she successfully obtained this degree and started afterwards in September 2021 the Master Psychosomatic Physiotherapy in Utrecht. Laura de Bruin sees importance in the provision of good quality care in an efficient and respectful manner that meets the preferences, wishes and expectations of a client as much as possible. In addition to individual treatments with clients, she supervises exercise groups. In recent years she has also followed several courses for headaches, neck-, shoulder- and back problems.
[Disclaimer: Please note that any recommendations and advice given on this website have been compiled with care. However, they are, in no way, meant to take the place of a medical doctor’s consultation and treatment. Should you have or assume to have a health-related problem, consult a medical professional and adhere to the medical advice provided, regardless of the information you have received on this website.
Should a serious injury have occurred, the diagnosis and treatment need to be provided by a medical specialist. If you are uncertain about the cause of your pain, it is advisable to also consult a medical professional.
If the medical symptoms are accompanied by reddening, swelling, overheating of the joints, persistent and serious pain and/or neurological symptoms (e.g. feeling of numbness, tingling), or if the pain extends to other parts of the leg, a medical professional needs to be consulted immediately.
The information on this website is not meant to constitute the basis for a self-diagnosis, treatment or medication.
Please always read carefully and adhere to the usage instructions or the pack insert of our Hansaplast products.
For further information on our products, please contact us on our Hansaplast hotline 040 / 4909 7570 (Mo.-Fr. 8.00 - 18.00h) or by email at Hansaplast@Beiersdorf.com.]









